Even though FHIR adoption has become more common among healthcare software providers, it's still tricky. Providers are sure to face different issues along the way. They must dig into specifications, ensure data consistency, care about security, and deal with other challenges.
Going through this process is easier with professional support and guidance from Binariks. Our company has already assisted multiple healthcare providers with FHIR adoption. In this guide, we share our expertise and explain what FHIR development involves.
What is FHIR?
In 2014, Health Level Seven International (HL7) implemented the FHIR standard to formulate data exchange rules in healthcare.
So what is FHIR in healthcare and how does FHIR work?
It's a new specification that guides healthcare software vendors on ensuring interoperability through APIs and connected data. Market leaders, including Allscripts, Cerner Corporation, Epic Systems Corporation, and others, have already adopted an API for the FHIR framework. These vendors cover 83% of hospitals or 58% of clinicians and keep overtaking the market.
The main idea behind FHIR is to simplify the adoption of EHR systems without compromising information integrity. When you follow the FHIR implementation guide, you use a trusted model of exchanging data between healthcare apps. As a result, your healthcare organization achieves the ultimate interoperability of its systems.
What does FHIR implementation mean for healthcare stakeholders
FHIR is a win-win story for patients, clinicians, healthcare providers, and other stakeholders. Despite requiring considerable investment, FHIR integration is worth it. It improves healthcare processes in many ways:
- FHIR healthcare standard for patients. Patients enjoy more data-driven and high-quality care. Interoperability also enables patients to quickly send their data while choosing an insurance plan and gives them better control over shared PHI.
- FHIR healthcare standard for health teams. The healthcare industry depends on easy access to health records. When they are available and understandable, teams can follow patients as they move through the healthcare ecosystem. Clinicians get a detailed patient profile and all healthcare app data in one place. It optimizes their work and eliminates the need to switch between many devices.
- FHIR healthcare standard for healthcare providers. FHIR makes healthcare providers compliant with industry standards, optimizes their work, and facilitates the transition to value-based care. Interoperability also enhances productivity, safeguards patient data, and increases ROI for EHR system.
- FHIR healthcare standard for developers. The FHIR standard facilitates interoperability since engineers have clear rules to rely on. They develop compliant healthcare systems that can process the data of individuals eligible for Medicare and Medicaid. As a result, these systems are suitable for a larger number of healthcare organizations, including those that must follow the Patient Access Final Rule.
FHIR components and resources
FHIR gives software developers a common way to build healthcare applications. If you know how the components of FHIR work, following its requirements is easier.
Here are the core FHIR resources and components to consider:
RESTful APIs
FHIR is a data API standards framework that allows developers to build apps with ready-made RESTful APIs. Software engineers can combine different FHIR standard resources to tailor the software to specific clinical use cases. Thanks to such pluggable solutions, developing a healthcare interoperability interface takes hours instead of days or weeks.
FHIR Profiles and Resources
Resources are the most critical aspects of the FHIR standard specification. These are any exchangeable content pieces, including a document, image, non-virtual object, etc. The primary function of resources is to exchange information between different EHR systems. For example, they may convey the patient's name, location, care plan, or family history.
FHIR profiles are closely related to resources. A profile is a set of rules that allows a FHIR standard resource to include extensions. Such a resource can add additional attributes and has a more specific definition.
Attributes
Attributes are resource-specific metadata included in FHIR resources. This data ensures that the framework is interpreted across systems and applications. FHIR resources are based on XML, HTTP, JSON, Atom, and OAuth.
Resource Data Formats
Since FHIR apps are developed from modular components, you need means to exchange and store data. Here are the elements FHIR resources must include:
- URL
- XHTML summary
- Metadata
- Definitions
- Managed extensibility framework specific to healthcare
FHIR integration process
FHIR may require profound changes in existing systems. The standard also imposes many strict requirements that are challenging to follow without a proper plan.
Thus, you must create a clear roadmap to deploy FHIR services and follow the best industry practices. You must also decide how FHIR resources will solve particular administrative or tech problems and develop the related documentation.
A clear FHIR integration process is essential to provide developers with the guidelines to follow. They will know how to achieve data interoperability and security required by the standard. It considerably facilitates the software development and implementation process. You will also avoid mistakes that can later hinder compliance.
Want to become HIPAA-compliant?
Learn about best practices of FHIR implementation.

Core types of FHIR implementation
The FHIR specification is quite a universal healthcare standard with many use cases. Some providers modify their systems only to become FHIR compliant. They don't view it as an opportunity to optimize their internal processes. Others build an entire data management process with third-party integrations and complex architecture. The differences in approaches affect the ways to implement an FHIR API.
Overall, there are two approaches FHIR creates:
Integrating FHIR API to an existing system
Since healthcare providers often have legacy systems, API integration on top of the current system is a standard option. In this case, the architecture of implementing FHIR consists of a database, data access layer, FHIR adapter, and FHIR API.
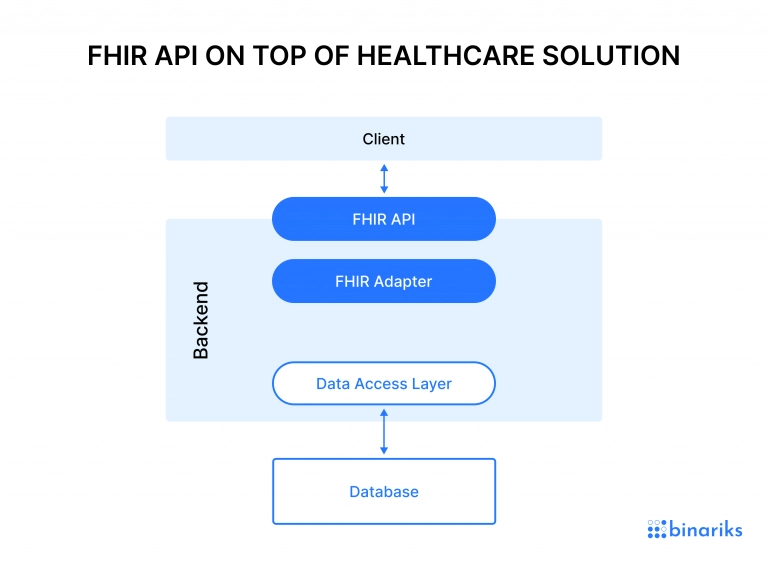
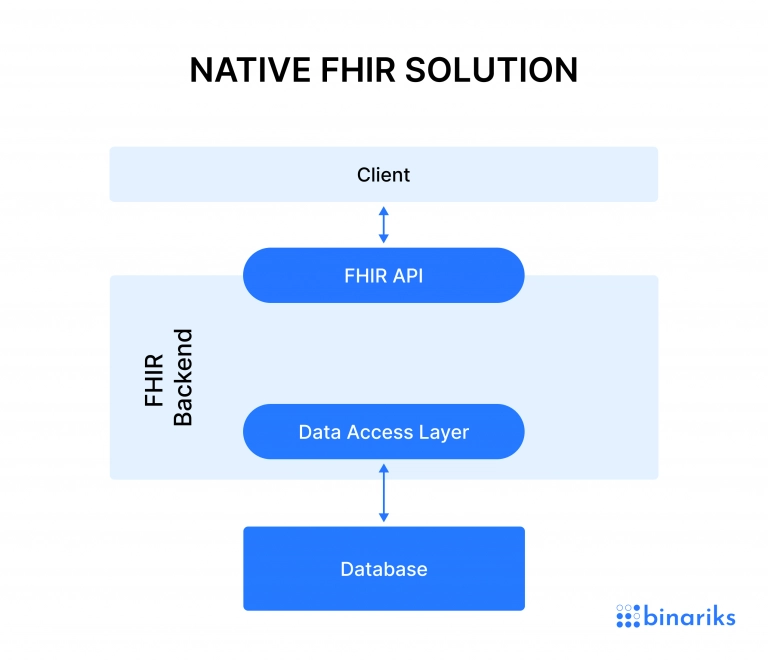
Native FHIR system
The native model is for healthcare organizations and software providers that create a system from scratch. Since FHIR compliance has already become an industry standard, every new product must be compatible with FHIR.
To achieve such compatibility, software developers must use FHIR resources, profiles, and extensions in software design. The FHIR resources will shape the proprietary data model and help build compatible interfaces and implementations.
Generally, the native FHIR approach is for the following cases:
- For new products and prototypes. FHIR delivers ready data models allowing startups to speed up software development while complying with the law.
- For data storage. FHIR provides you with data storage and processing capabilities you can use to create temporary storage or instead of building an adapter.
If you doubt which model is suitable for you, contact Binariks for consulting or practical assistance.
SMART on FHIR
If you seek ways to implement FHIR, SMART can facilitate the process. SMART is an open-source API that leverages OAuth 2.0 to provide universal access to EHRs. It builds on the existing FHIR resources and, therefore, is called SMART on FHIR .
When combined, SMART and FHIR offer everything a software engineer needs to build an app that will run anywhere in the healthcare system. The universality of SMART enables providers to customize apps on an individual level. It eliminates the need to use the same apps within a healthcare system while allowing everyone to exchange data without obstacles.
Read more about implementing SMART on FHIR in the related article by Binariks.
How is FHIR different from HL7?
Healthcare providers and software companies researching FHIR compliance often confuse it with HL7. Now that we've discussed all you need to know about FHIR let's talk about HL7.
The term HL7 stands either for the Health Level Seven International organization that formulates healthcare standards or a set of international standards it has launched. The HL7 standards set a clinical messaging format for the secure exchange of communications and documents between healthcare organizations.
So what's the difference?
The HL7 V2 and V3 create a foundation for FHIR as a more modern alternative to the existing HL7 standards. FHIR includes many previous HL7 requirements but employs RESTful web services and open web technologies, including not only XML but also RDF and JSON data formats. These technologies are more popular, which allows a larger number of developers to leverage the FHIR's potential. This way, while HL7 mainly improves interoperability, FHIR also streamlines the implementation of interoperable software systems.
Validation error:
The selected type is invalid.
6 FHIR healthcare standard implementation challenges you may face
Regardless of the FHIR implementation model you adopt, be sure to brace yourself for challenges. Since FHIR healthcare standards are a new thing, there are no visible FHIR API implementation case studies. It may be difficult to predict what can go wrong and how to deal with the consequences.
Here we have collected six FHIR healthcare service challenges that happen the most often.
#1. FHIR-compliant systems take time and resources
If you are about to start FHIR implementation, prepare for a lengthy process. You will need to go through many stages, from foundational to structural interoperability. Foundational interoperability of FHIR-compliant systems means that you need to meet inter-connectivity requirements in every app you use. Applications must securely exchange data and communicate. Organizational interoperability involves structural changes. Every end-user process and communication between organizations, entities, and individuals must be integrated.
Simply put, FHIR implementation requires a profound analysis of the existing software. You will need to invest in quality research of your current systems to upgrade them. It strains resources but helps to build FHIR healthcare services with the highest level of interoperability.
#2. You have to tailor FHIR integration to specific business needs
Apart from technical optimization, FHIR-compliant systems pursue business goals. Hence, FHIR implementations require skilled business analysts. It's particularly true for healthcare TPAs. Whereas the demands of traditional healthcare providers overlap, third-party actors have unique business logic and healthcare data uses. For example, they may need to join patient health records and insurance data in a single system. Hence, a technology partner that offers a data exchange system for such an organization will need to research its business logic and data types before building data infrastructure. It creates additional HL7 FHIR integration service challenges.
#3. FHIR security issues are unavoidable
Even if you are HIPAA-compliant and protect patient data, FHIR will make you rethink some security practices. The thing is that when adopting FHIR healthcare services, you need to share access to some data stored in your systems. It increases vulnerability and results in additional security challenges. Interoperability raises questions about how to map data but maintain the same privacy of exchanged data as with other PHI. You will need the multi-tenant model with rich use functions, responsibilities, and permissions. It gives better control over data but is also more difficult to configure.
#4. Lack of technical expertise
To adopt FHIR services, healthcare vendors and TPAs need either skilled in-house specialists or external help for FHIR development. Since HL7 FHIR services are a relatively fresh standard, the number of people who know how to implement FHIR cloud platforms is limited. Hence, if you start to look for FHIR API proficient engineers, you will face a shortage. Currently, the number of healthcare entities that strive to meet FHIR requirements is increasing, and the demand for FHIR APIs specialists is tremendous.
That's why finding someone to implement FHIR services may be a challenge. Most healthcare companies consider hiring an external vendor as a way to overcome it. A software development agency with relevant experience can create custom open-source solutions meeting FHIR requirements time- and cost-efficiently.
#5. Data consistency across third-party software
Data manageability and consistency are critical for setting up FHIR APIs functionality. The records across connected third-party software must have the same format and match. Only then will you achieve interoperability of cloud FHIR solutions. Building a system with consistent data or moving Epic to the cloud is much more challenging than it might seem. You will have to analyze potential data issues, develop data processing rules, define compliance metrics, implement data remediation procedures, and more. Read also: How to Integrate an EHR system like Epic, Cerner or MEDITECH.
#6. FHIR integration process is a never-ending story
In the future, healthcare systems will only get more complicated. Besides, the FHIR standard is not compatible with every system. Hence, you will have to test the data sharing practices in third-party apps you connect to maintain FHIR security and stay HIPAA-compliant.
Hence, hiring a professional FHIR provider may be the best way out. They will provide ongoing support and help you adopt new features while staying compliant.
How Binariks facilitates FHIR implementation
Binariks is a software development provider with experienced FHIR experts that designs software for healthcare companies. We are building HIPAA-compliant software and can implement CMS interoperability in healthcare based on the latest FHIR standards.
We can help you comply with FHIR in the following ways:
- Consult you on FHIR adoption after researching your business case
- Outstaff our software engineers proficient in FHIR solutions to help you meet the requirements of the standard
- Assemble a dedicated team for you to develop a custom healthcare solution that complies with FHIR, HIPAA, and other industry-specific regulations.
Check out the projects Binariks has completed here to learn more about how we work.
Final thoughts
FHIR for healthcare software developers entails a range of challenges. It takes effort to master new data interoperability standards and find the best approaches to implement them. Healthcare services and TPAs also need to ensure data security and tailor FHIR services to business needs. Nonetheless, the benefits of FHIR overpower the challenges and yield great results in the long run. A healthcare organization becomes more productive and the quality of care significantly improves.
If you need help with integrating API for the FHIR framework , Binariks is ready to assist you. Contact us to discuss your case and get a reliable tech partner.
FAQ
Share

