Artificial intelligence in medical imaging refers to the use of machine learning, deep learning, and computer vision techniques to analyze medical images and support clinical decision-making. Instead of relying solely on manual image interpretation, AI systems assist radiologists and clinicians by detecting patterns, highlighting anomalies, and prioritizing cases within diagnostic workflows.
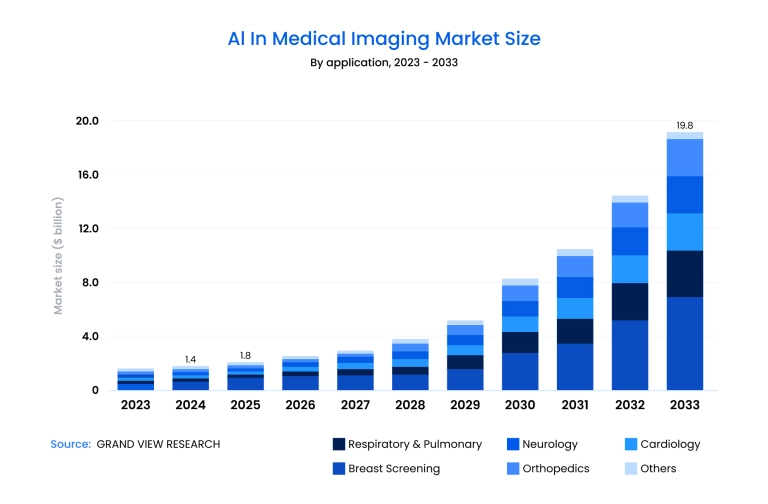
From a market perspective, the impact is already measurable. According to Grand View Research, the global artificial intelligence (AI) in the medical imaging market was valued at USD 1.36 billion in 2024 and is projected to reach USD 19.78 billion by 2033, growing at a CAGR of 34.67% from 2025 to 2033.
The rising demand for early and accurate diagnosis, the increasing volume of imaging data, and rapid advances in AI and ML technologies are the primary drivers of this growth.
In practical terms, AI-based medical imaging has become a foundational capability for modern healthcare workflows. It supports faster diagnostics, improves consistency of image interpretation, and helps healthcare providers manage growing workloads more effectively.
Its adoption also reflects broader industry momentum, as seen in the growth of AI in healthcare , where intelligent systems are embedded directly into clinical and operational processes.
This article covers:
- How AI fits into end-to-end medical imaging workflows, from image acquisition to diagnosis
- Why AI adoption in medical imaging is accelerating across hospitals and diagnostic centers
- Which core technologies enable AI-driven image analysis and clinical support
- Where AI delivers the most clinical and operational value today
- What challenges healthcare organizations face when integrating AI into imaging workflows
Continue reading to explore how these technologies reshape diagnostics, clinical efficiency, and healthcare delivery in practice. The following sections break down the evolution, applications, and real-world impact of AI in medical imaging.
The evolution of medical diagnostics: From manual analysis to AI
Before the use of AI in medical imaging, diagnostic workflows were built almost entirely around manual interpretation and human expertise.
Image acquisition required technicians to make precise adjustments to the imaging equipment, while radiologists visually inspected X-rays, CT scans, and MRIs to identify abnormalities. Measurements such as lesion size, organ volume, or structural changes were performed manually, increasing analysis time and introducing variability.
These workflows were inherently difficult to scale. Growing imaging volumes placed sustained pressure on radiology teams, leading to fatigue, inconsistent interpretation quality, and delayed prioritization of urgent cases. Subtle patterns linked to early-stage disease progression were often hard to detect, limiting the predictive diagnostics and early intervention.
The shift toward AI-assisted diagnostics addresses these structural limitations. By introducing automated pattern recognition, image quantification, and decision support, modern systems reduce dependence on subjective judgment while improving consistency across providers.
This evolution is closely tied to advances in computer vision in medical imaging , which enable machines to analyze visual data at speeds and with precision that manual workflows cannot match.
Today, AI-driven imaging is increasingly relevant beyond specialized radiology departments. The growing role of AI in primary care imaging reflects how diagnostic support tools are extending into earlier stages of patient care, helping clinicians manage imaging workloads, identify risks sooner, and make more informed referral decisions.
This transition from manual analysis to AI-assisted workflows marks a structural change in how medical imaging supports diagnosis, scale, and clinical decision-making across healthcare systems.
AI in medical imaging: Market growth and adoption
The rapid adoption of artificial intelligence and medical imaging is closely tied to structural changes in how diagnostic services are delivered. Healthcare systems are processing more imaging studies per patient, across more modalities, with higher expectations for speed and consistency. AI adoption reflects a response to these pressures rather than purely technological enthusiasm.

What is driving market adoption today
Healthcare providers are increasingly deploying AI in imaging workflows to address operational and clinical bottlenecks that manual diagnostics struggle to resolve at scale. The strongest adoption signals come from hospital networks and imaging centers integrating AI directly into existing PACS and cloud-based infrastructures.
Key factors accelerating adoption include:
- Persistent shortages of qualified radiologists and growing diagnostic workloads
- Rising demand for early detection in oncology, neurology, and cardiovascular care
- The need to standardize image interpretation quality across teams and locations
- Faster turnaround expectations for both routine and urgent imaging studies
- Increasing reliance on automated imaging with minimal training required to lower implementation barriers
From a technical standpoint, deep learning remains the dominant approach due to its effectiveness in complex image analysis tasks. The continued expansion of the artificial intelligence in MRI market reflects how AI is used not only for detection but also for image reconstruction, noise reduction, and workflow optimization in data-intensive modalities.
Regional and organizational adoption patterns
Adoption patterns show clear regional differences. North America leads in enterprise-scale deployments due to established digital infrastructure and regulatory readiness, while Asia-Pacific demonstrates the fastest growth driven by large-scale healthcare digitization initiatives. Across regions, AI is increasingly deployed as part of orchestrated clinical systems rather than isolated diagnostic tools.
The current stage of market growth is defined by integration depth. AI in medical imaging is moving beyond assistive diagnostics toward embedded decision support within coordinated clinical workflows. This aligns imaging AI with broader automation strategies such as agentic AI workflows in healthcare , where AI systems contribute to prioritization, routing, and clinical coordination.
Overall, market adoption signals a transition from experimental usage to operational dependence, positioning AI in medical imaging as a foundational capability for scalable, high-quality diagnostics.
Core technologies behind AI in medical imaging
AI in medical imaging is built on a set of tightly connected technologies that together enable reliable image analysis, clinical decision support, and scalable deployment across healthcare workflows. These sub-entities form the technical foundation of modern imaging systems and directly support AI in medical imaging diagnosis across modalities.
Computer vision in medical imaging
Computer Vision is the core technology that allows systems to interpret medical images as structured visual data. It enables the detection of anatomical structures, abnormalities, and spatial relationships within X-rays, CT scans, MRIs, and ultrasound images.
By translating pixels into clinically meaningful features, computer vision acts as the backbone of image-based automation and supports an AI-optimized radiology workflow that integrates directly into diagnostic pipelines. In production environments, these capabilities are typically developed and fine-tuned through enterprise-grade AI/ML development practices to ensure accuracy, scalability, and compliance.
Deep learning for image analysis
Deep learning drives the most advanced image analysis tasks in medical imaging. Neural networks, particularly convolutional architectures, excel at recognizing complex patterns, segmenting images, and classifying findings across large imaging datasets.
These models improve diagnostic consistency by learning subtle visual cues that are difficult to detect through manual analysis alone, especially in oncology, neurology, and cardiovascular imaging.
Machine learning in diagnostic support
Machine learning underpins decision support by enabling models to learn from historical imaging data, clinical labels, and outcomes.
ML techniques support risk stratification, prioritization of imaging studies, and predictive insights that assist clinicians rather than replace them. By continuously learning from new data, machine learning systems help maintain diagnostic relevance as imaging volumes, protocols, and patient populations evolve.
Together, these technologies form a cohesive foundation that allows AI in medical imaging to move from isolated image analysis toward integrated, workflow-driven clinical support.
Applications of AI in medical imaging
The practical value of medical imaging and AI becomes most visible when applied to specific clinical scenarios. Across diagnostic domains, AI supports faster interpretation, higher consistency, and earlier detection by embedding intelligence directly into the AI radiology workflow rather than operating as a separate analytical layer.
Cardiovascular conditions
In cardiovascular imaging, AI assists with automated chamber segmentation, functional assessment, and early risk indicators derived from echocardiography, CT, and X-ray data. Algorithms can flag structural changes such as atrial enlargement or valve abnormalities, helping clinicians identify cardiac conditions earlier and prioritize patients who require immediate follow-up.
Neurological conditions
AI plays a critical role in neurology by analyzing brain imaging data to detect subtle patterns associated with neurodegenerative diseases. In conditions such as Alzheimer’s or ALS, models support earlier diagnosis by identifying metabolic or structural changes that are difficult to recognize through manual review, enabling better long-term care planning and disease monitoring.
Cancer screening
In cancer screening, AI improves sensitivity and reduces false positives across modalities such as mammography, colonoscopy imaging, and CT scans. By detecting microcalcifications, lesions, or polyps at early stages, AI supports more reliable screening programs and helps clinicians intervene before disease progression accelerates.
Brain tumors
For brain tumor analysis, AI models assist with tumor detection, classification, and segmentation using MRI data. These systems can differentiate tumor types, assess growth patterns, and support non-invasive diagnostic pathways, reducing reliance on risky procedures while improving diagnostic confidence.
Fractures and musculoskeletal injuries
In musculoskeletal imaging, AI enhances fracture detection by identifying subtle bone injuries that may be missed during routine interpretation. This is particularly valuable for spinal and hip fractures, where delayed diagnosis can lead to serious complications, especially in elderly or trauma patients.
Together, these use cases illustrate how AI in medical imaging translates from technical capability into clinical impact, supporting diagnostic accuracy and workflow efficiency across diverse medical domains.
Real-world examples of AI in medical imaging
AI in medical imaging is already deployed in clinical environments where diagnostic speed, accuracy, and scalability directly affect patient outcomes. The following cases come from healthcare institutions, public health systems, and academic research, demonstrating real-world adoption beyond experimental settings.
AI-assisted stroke detection in emergency CT imaging (United States)
Hospitals in the US increasingly rely on AI-assisted triage systems to analyze non-contrast head CT scans for signs of stroke and intracranial hemorrhage. These systems automatically flag suspected abnormalities and prioritize urgent cases for radiologist review.
Clinical studies show meaningful reductions in reporting time and improved diagnostic confidence, particularly in emergency and high-volume settings.
AI in breast cancer screening programs (United Kingdom)
In breast cancer screening, AI is being integrated as a decision-support tool within national healthcare workflows rather than as a standalone diagnostic system.
A notable example is the NHS-led EDITH trial in the UK, a large randomized controlled study involving approximately 660,000 women across 30 screening centers that evaluates how AI can assist expert interpretation of mammograms.
The trial assesses AI used both as a secondary reader and as a triage mechanism to prioritize high- and low-risk cases, while keeping final decisions with human experts. Its focus on detection rates, recall balance, and cost-effectiveness demonstrates how AI can enhance large-scale screening programs without compromising clinical governance.
Brain tumor detection and classification
AI is increasingly used to support brain tumor detection and classification by analyzing MRI scans with high consistency and speed. Recent peer-reviewed research demonstrates that deep learning models trained on large, standardized MRI datasets can accurately distinguish between tumor and non-tumor images while reducing variability caused by human interpretation.
In clinical practice, this translates into faster preliminary assessments, more consistent identification of subtle abnormalities, and stronger decision support for radiologists, particularly in high-volume or complex diagnostic scenarios where early and reliable tumor detection is critical.
Overall, these use cases show how AI in medical imaging moves beyond theoretical value into measurable clinical impact, supporting earlier detection, more consistent interpretation, and more efficient radiology workflows across diverse diagnostic domains.
Key advantages of AI in medical imaging
Large-scale clinical studies and industry research show measurable gains in diagnostic accuracy, operational efficiency, and care delivery when AI is embedded into real imaging workflows rather than used as standalone tools.
1. Improved diagnostic accuracy
Peer-reviewed research confirms that AI systems trained on large imaging datasets can detect clinically relevant patterns that are difficult to identify through visual inspection alone.
A comprehensive review published in PubMed , shows that deep learning models significantly improve detection of tumors, vascular abnormalities, retinal disease, and neurological conditions by identifying subtle structural and textural features. Earlier detection directly improves treatment options and patient outcomes, particularly in oncology and cardiovascular care.
2. Increased efficiency
Radiology departments are under sustained pressure from growing imaging volumes and staff shortages.
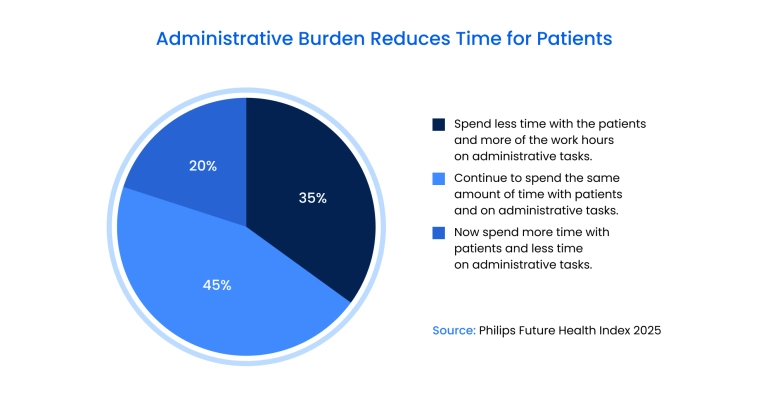
According to the Philips Future Health Index 2025 , over 35% of healthcare professionals now spend less time with patients due to administrative and operational workload. AI reduces scan acquisition time, accelerates image reconstruction, and shortens interpretation cycles, allowing departments to process more studies without compromising diagnostic quality.
3. Enhanced clinical workflows
AI supports the entire imaging pipeline, from acquisition and preprocessing to interpretation and reporting. Automated segmentation, standardized measurements, and intelligent case prioritization reduce variability between clinicians and improve turnaround times.
Evidence summarized in the Springer Nature highlights how AI-driven workflows improve consistency across CT, MRI, and PET imaging, particularly in high-volume hospital environments.
4. Cost-effectiveness
Operational efficiency translates directly into financial impact. Faster exams, fewer repeat scans, and optimized staff utilization reduce per-case costs.
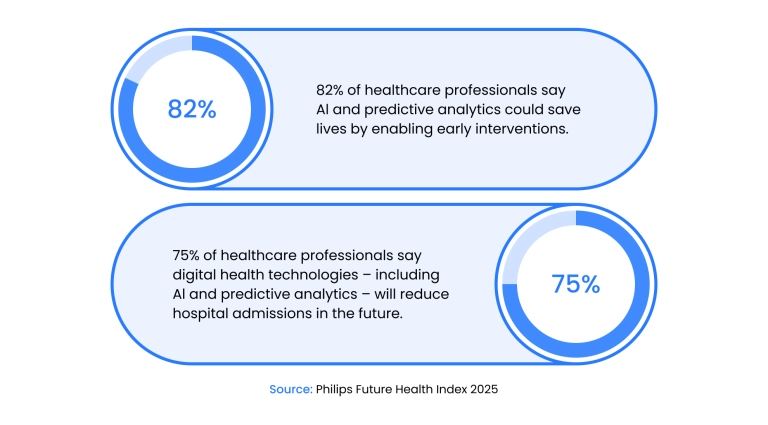
The Philips Future Health Index reports that 75% of healthcare professionals believe AI and predictive analytics will reduce hospital admissions over time, driven by earlier detection and better triage. Lower rates of late-stage diagnosis also reduce downstream treatment costs.
5. Consistent quality of analysis
Human interpretation is inherently influenced by workload, fatigue, and experience level. AI delivers reproducible results across shifts, locations, and patient populations.
Machine-learning-based analysis ensures consistent image quality assessment and measurement accuracy, which is especially critical for national screening programs and multi-center clinical networks.
6. Advanced diagnostic capabilities
AI enables diagnostic capabilities that were previously difficult to scale. Deep learning models support precise image segmentation, quantitative biomarker extraction, longitudinal disease tracking, and personalized treatment planning.
AI-assisted imaging allows clinicians to correlate imaging features with patient-specific risk profiles, supporting more targeted and proactive care decisions.
Complementary technologies that enhance AI in medical imaging
AI in medical imaging does not operate in isolation. Its real impact emerges when combined with adjacent technologies that extend analytical depth, clinical usability, and system scalability across healthcare environments.
Big data and multimodal imaging repositories
Modern imaging AI depends on access to large, diverse datasets that combine scans with clinical records, lab results, and longitudinal patient history. This data foundation enables stronger validation, reduces bias, and supports population-scale learning, as reflected in AI-assisted radiology market trends.
Cloud and edge computing infrastructure
Cloud platforms support large-scale model training and continuous updates, while edge computing enables real-time inference directly on scanners and imaging devices. This hybrid architecture improves latency, data security, and compliance in hospital environments.
3D imaging, AR, and VR technologies
AI-enhanced 3D reconstruction, augmented reality, and virtual reality are expanding beyond visualization into surgical planning, interventional radiology, and clinician training. These tools translate AI outputs into spatial, actionable insights.
Connected medical devices and wearables
Imaging AI increasingly integrates with data from smart medical devices and wearables. When imaging findings are combined with continuous physiological data, providers gain a more complete picture of disease progression and treatment response.
Augmented intelligence for clinicians
Rather than replacing clinicians, AI systems are embedded into diagnostic workflows as decision-support tools. Case prioritization, anomaly highlighting, and standardized measurements improve consistency while keeping final decisions with medical professionals.
Interoperability and standards-based integration
Standards such as DICOM, HL7, and FHIR enable AI solutions to integrate with PACS, RIS, and hospital information systems. This interoperability is a critical enabler for scaling artificial intelligence in the medical imaging market without disrupting existing clinical operations.
Challenges of AI integration in medical imaging and how to address them
| Challenge | Core Problem | Practical Solution |
| System compatibility | Legacy PACS, RIS, and EHR systems are not designed for native AI integration, making deployment slow and expensive | Use middleware and standards-based integration layers to connect AI tools without replacing existing infrastructure |
| Data quality and labeling | Medical imaging datasets are inconsistent, incomplete, or poorly labeled, reducing model accuracy | Implement standardized data pipelines, semi-automated labeling, and continuous dataset validation |
| Alignment with clinical decision-making | AI outputs are probabilistic and may not match clinical guidelines or physician judgment | Position AI as decision support only and train models using real-world clinical workflows and outcomes |
| Bias, reliability, and security | Models may inherit demographic bias and expose sensitive imaging data to cyber risks | Train on diverse datasets, monitor performance across populations, and enforce strong encryption and access controls |
| Implementation and maintenance costs | High upfront costs, staff training needs, and ongoing model retraining slow adoption | Start with focused use cases, validate ROI early, and plan continuous updates as part of operational budgets |
| Ethical and legal accountability | Responsibility for AI-assisted diagnostic decisions is often unclear | Define governance frameworks that ensure human oversight, explainability, and accountability |
AI delivers clear value in medical imaging, but adoption comes with predictable technical, operational, and regulatory challenges. The key is addressing them systematically rather than treating AI as a plug-and-play tool.
Will adopting GenAI mark the next chapter for your business?
Download our free whitepaper now to find out.

Our experience in AI and medical imaging solutions
Binariks develops production-grade computer vision in medical imaging systems that integrate into clinical workflows and meet healthcare compliance requirements. Our work spans the full development lifecycle: from annotated dataset preparation and model architecture selection to HIPAA-compliant deployment within hospital infrastructure.
Our AI/ML development practice for healthcare focuses on:
- Medical video and image analysis: We build custom computer vision models for real-time surgical scene recognition, diagnostic image classification, and anomaly detection across CT, MRI, and video modalities.
- Healthcare system integration: Our solutions connect with PACS, RIS, and EHR environments through standards-based APIs (DICOM, HL7 FHIR), ensuring AI tools augment rather than disrupt existing radiology workflows.
- Scalable cloud infrastructure: We deploy models on AWS (SageMaker, EC2) and design hybrid cloud-edge architectures that balance inference speed, data security, and regulatory compliance.
- Model validation and monitoring: Our teams implement MLflow-based experiment tracking, continuous performance monitoring across patient populations, and bias detection frameworks to maintain diagnostic reliability.
Binariks' case study: AI-powered surgical scene recognition
A recent engagement demonstrates our approach to healthcare AI in practice. Working with a UK-based healthcare platform provider used by 800+ hospitals globally, we developed a real-time surgical video recognition solution to optimize operating room (OR) efficiency.
Technical challenge
Build a computer vision system capable of identifying critical surgical milestones—procedure start, completion, and OR readiness—from live video streams to reduce downtime and improve scheduling accuracy.
Our solution
- Model architecture research: Evaluated MoviNets, TSM, 3DCNN, and TimeSformer on 500+ hours of annotated surgical videos. Selected TimeSformer for its transformer-based temporal analysis and superior accuracy-efficiency balance.
- Custom training pipeline: Fine-tuned models using PyTorch on AWS EC2 GPU instances, achieving 82% event classification accuracy with a roadmap to 95%.
- Production deployment: Implemented real-time inference via AWS SageMaker with GStreamer video processing, enabling hospitals to monitor OR utilization and optimize scheduling in real time.
- Scalable infrastructure: Built CI/CD pipelines using Docker and Git for continuous model updates, ensuring the system evolves as more labeled surgical data becomes available.
Clinical impact
The solution now supports hospital OR effectiveness (ORE) analytics, reduces patient wait times through better scheduling, and provides data-driven insights for process optimization – demonstrating how AI in medical imaging translates from technical capability into measurable operational value.
This project reflects our broader expertise across the artificial intelligence in the medical imaging market, including work on diagnostic image analysis, workflow automation, and regulatory-compliant AI deployment. For healthcare organizations moving from pilots to production, our teams design systems that integrate with existing clinical infrastructure, comply with data security standards, and deliver validated performance across diverse patient populations.
Final thoughts
AI in medical imaging has evolved from experimental technology to strategic infrastructure. With the market projected to reach USD 19.78 billion by 2033, healthcare organizations now deploy AI to improve diagnostic accuracy, optimize workflows, and scale capacity under growing imaging volumes.
Production success requires systems that integrate with existing infrastructure, maintain regulatory compliance, and deliver validated clinical outcomes, not just lab-tested models.
Binariks develops AI-powered medical imaging solutions that work in real clinical environments. From model training to HIPAA-compliant deployment, we help healthcare providers and healthtech companies move from pilots to production with measurable impact.
Ready to optimize your imaging workflows? Contact Binariks to discuss how computer vision in medical imaging can be applied to your diagnostic processes.
Share

